Prior authorization remains one of the most significant administrative bottlenecks for specialty practices today, often leading to treatment delays and lost revenue. Outsourcing this complex task to a specialized partner can reclaim hundreds of staff hours and improve your practice's
Why Practices Are Outsourcing Prior Authorization
Prior authorization is the process by which insurance payers determine the medical necessity of a service or medication before it is provided. According to the American Medical Association, this process is a leading cause of administrative burden, often requiring hours of phone time and complex documentation. As specialty practices face increasing pressure to maintain patient care standards, many are turning to third-party RCM (Revenue Cycle Management) partners to manage these workflows. Outsourcing allows practices to leverage specialized expertise, reduce denial rates, and ensure that patient care is not delayed by insurance red tape.
How We Vetted These Providers
We evaluated these providers based on four key metrics: specialty-specific expertise (their ability to handle complex clinical documentation), EHR integration capabilities, transparency of reporting, and cost structures. We prioritized firms that offer dedicated account management and demonstrable improvements in approval turnaround times. Our selection process excluded generalist staffing agencies, focusing instead on organizations with a proven track record in medical revenue cycle management.
Here is a quick look at the top-rated prior authorization outsourcing services for 2026.
| Provider | Best For | Pricing |
|---|---|---|
| Verityx Health Access Solutions | Specialty Practices | Custom quote |
| DrCatalyst | Large-scale RCM Integration | Hourly rates starting at $13-$14/hr |
| CureMD | Flexible Scalability | Customized plans based on collections or volume |
| RCM Experts | Denial Management and Appeals | Custom quote based on monthly claim volume |
| AuthNet | Process Optimization | Custom quote |
The 5 Best Prior Authorization Outsourcing Services in 2026
#1 Verityx Health Access Solutions
 A screenshot of the Verityx Health Access Solutions website.
A screenshot of the Verityx Health Access Solutions website.
Verityx Health Access Solutions offers a targeted, HIPAA-compliant approach specifically designed for specialty clinics, including Rheumatology, Gastroenterology, and Oncology. They specialize in managing high-volume authorization workflows and benefits investigations, integrating directly with payer portals like CoverMyMeds to streamline requests. By offloading administrative bottlenecks to their remote team, practices can maintain clinical continuity without needing to hire additional in-house staff. Their focus on operational agility makes them a strong partner for practices looking to reduce administrative fatigue while improving approval times.
Provider Breakdown:
- Pro: Deep expertise in complex, high-volume specialty medication workflows.
- Con: Limited to specific specialty clinic environments.
- Pricing: Custom quote
#2 DrCatalyst
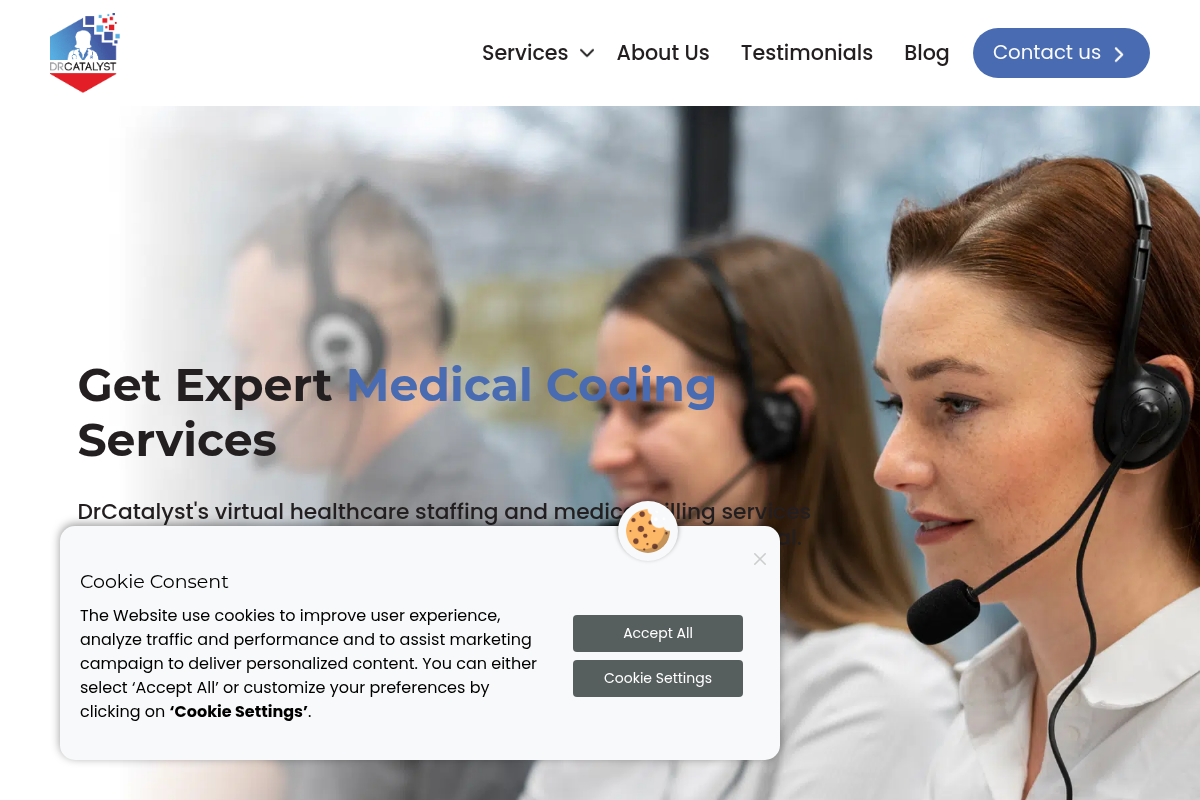 A screenshot of the DrCatalyst website.
A screenshot of the DrCatalyst website.
DrCatalyst provides comprehensive RCM services, including a robust prior authorization division that handles over 40,000 monthly requests across 60+ specialties. Their model utilizes US-based account managers paired with offshore billing teams, offering a multi-tiered supervision structure that ensures accuracy. They integrate deeply with existing EHR and practice management systems, providing transparent daily productivity reports. While they offer a wide range of services, their pricing is typically structured around hourly rates for dedicated staff.
Provider Breakdown:
- Pro: Extensive integration capabilities with over 60 different EHR platforms.
- Con: Requires long-term service agreements (6-12 months).
- Pricing: Hourly rates starting at $13-$14/hr
#3 CureMD
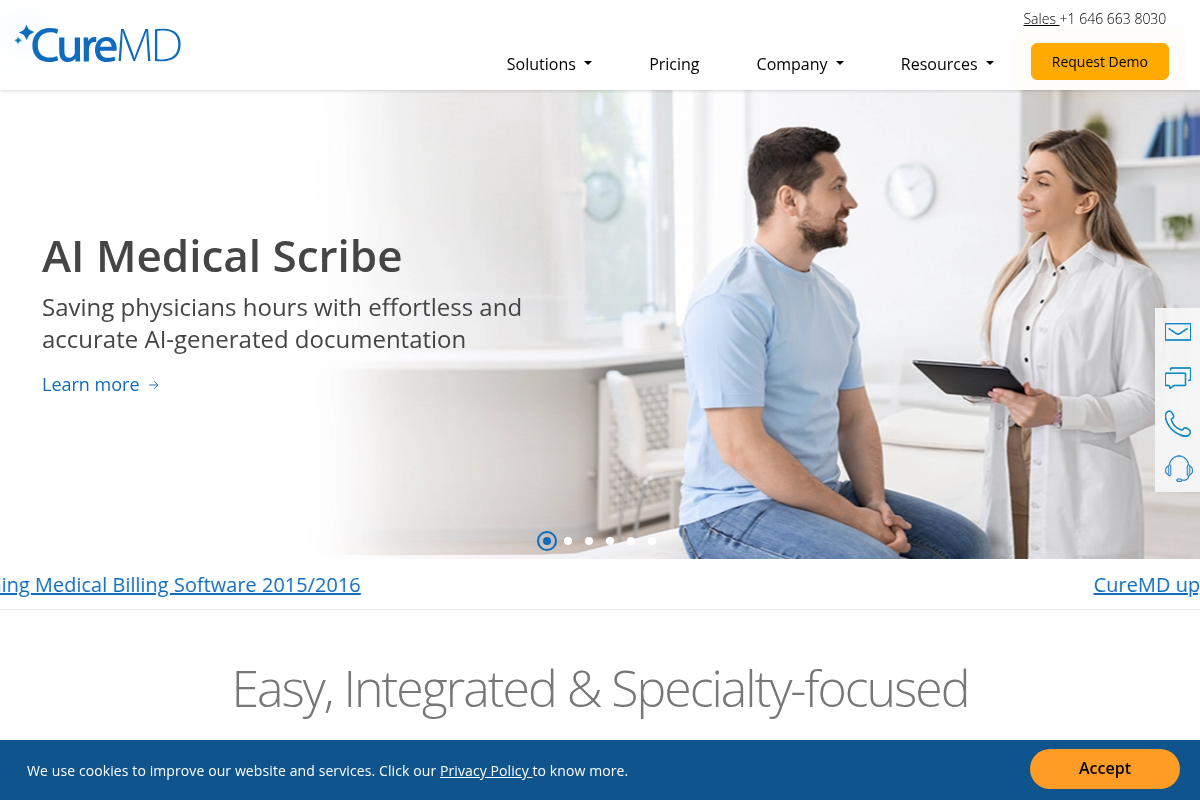 A screenshot of the CureMD website.
A screenshot of the CureMD website.
CureMD is a well-established player in the medical billing and practice management space, offering end-to-end prior authorization support. Their service is designed to be scalable, making it suitable for both solo practitioners and larger medical groups. They emphasize fast turnaround times—often securing approvals in under 48 hours—and provide real-time status updates through their platform. Their pricing models are highly flexible, ranging from percentage-of-collections to per-provider monthly fees, allowing practices to choose what fits their budget.
Provider Breakdown:
- Pro: Proven track record of securing approvals within 48 hours.
- Con: Support for non-CureMD EHR users can be more complex.
- Pricing: Customized plans based on collections or volume
#4 RCM Experts
 A screenshot of the RCM Experts website.
A screenshot of the RCM Experts website.
RCM Experts focuses heavily on the documentation-heavy side of prior authorization, including medical necessity validation and complex appeals. They provide a structured workflow that includes insurance eligibility verification before submission, which helps prevent wasted effort on non-covered services. Their team is trained to handle payer-specific protocols for a wide variety of specialties, from dermatology to neurosurgery. They are particularly popular with practices that struggle with high denial rates due to incomplete clinical notes.
Provider Breakdown:
- Pro: Strong focus on gathering clinical notes to ensure high approval rates.
- Con: Primarily focused on RCM-heavy workflows rather than general administrative support.
- Pricing: Custom quote based on monthly claim volume
#5 AuthNet
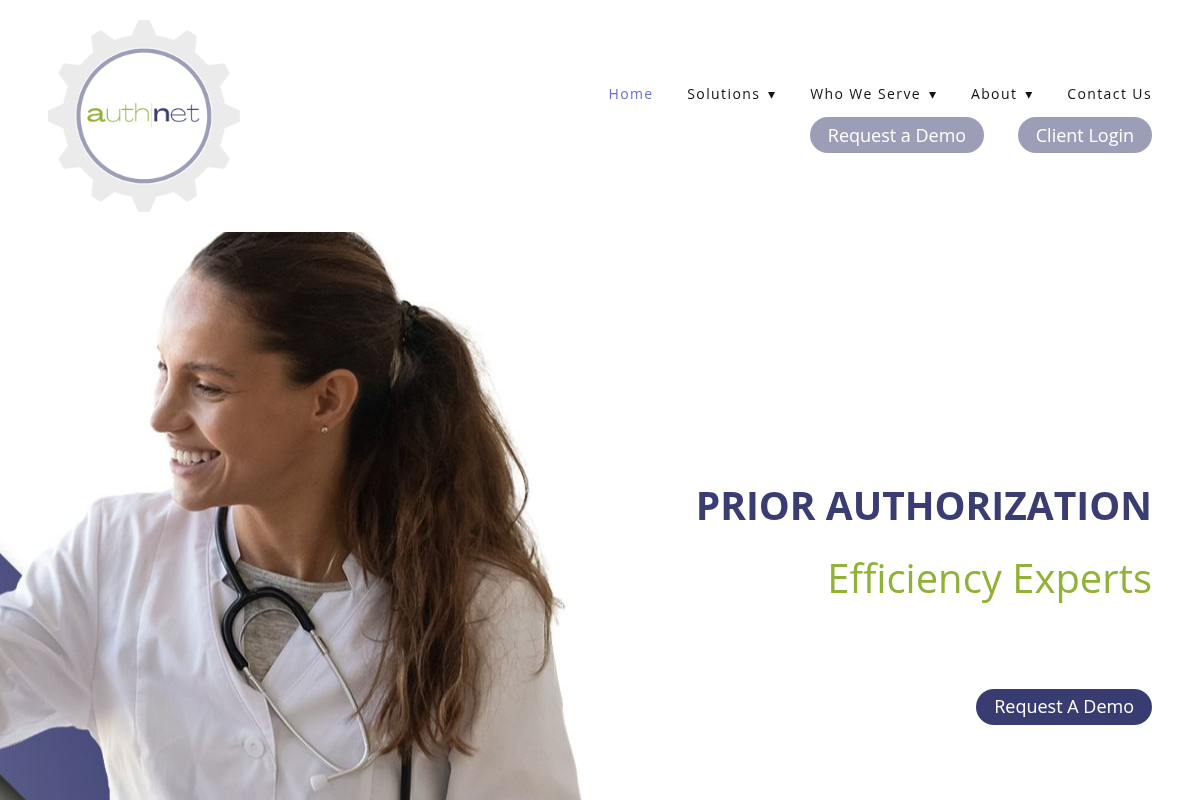 A screenshot of the AuthNet website.
A screenshot of the AuthNet website.
AuthNet specializes in insurance precertification and authorization services, positioning themselves as efficiency experts for hospitals and ambulatory practices. They provide a streamlined process that updates records directly within the practice's billing system, ensuring that the entire revenue cycle remains synchronized. Their service is built to handle the constant changes in payer policies, which takes the burden of training off of the practice's internal staff. They often provide ROI analyses to help practices understand the specific cost savings of outsourcing versus in-house processing.
Provider Breakdown:
- Pro: Provides clear ROI analysis to demonstrate potential cost savings.
- Con: Less emphasis on broader EHR integration compared to larger RCM firms.
- Pricing: Custom quote
Selecting the Right Partner
When evaluating these providers, prioritize those that offer a clear understanding of your specific clinical specialty. Ask potential partners about their experience with your specific EHR and how they handle the appeals process when a denial occurs. Transparency is non-negotiable; ensure the provider offers real-time tracking of authorization requests so your staff always has visibility into the status of patient procedures.
Automating Your Workflow
While human expertise is crucial for complex clinical documentation, look for partners that leverage AI-driven data entry and automated portal submissions. This combination reduces manual errors and accelerates the time it takes to get a response from insurance payers. The most efficient workflows combine these automated tools with dedicated specialists who can handle the nuances of peer-to-peer reviews and complex clinical justifications.
The Verdict
Outsourcing your prior authorization process is no longer just a cost-saving measure; it is a strategic necessity for specialty practices aiming to improve patient outcomes and reduce administrative burnout. By selecting a partner that aligns with your practice size and clinical specialty, you can transform a major operational headache into a streamlined, revenue-protecting asset. Start by requesting a demo or an ROI analysis from your top two choices to see how their workflow meshes with your existing system.

